Upgrade Rate and Associated Predictive Factors of Papillary Breast Lesions on Core Needle Biopsy in a Private Tertiary Institution:
A Cross-sectional Study
DOI:
https://doi.org/10.21141/PJP.2025.06Keywords:
papilloma, papillary breast lesions, upgrade rate, core needle biopsyAbstract
Objective. The aim of this study was to determine the upgrade rate in diagnosis of biopsy-proven papillary breast lesions on core needle biopsy and their respective surgical excisions, and to assess for predictive factors associated with an upgrade at St. Luke’s Medical Center – Global City.
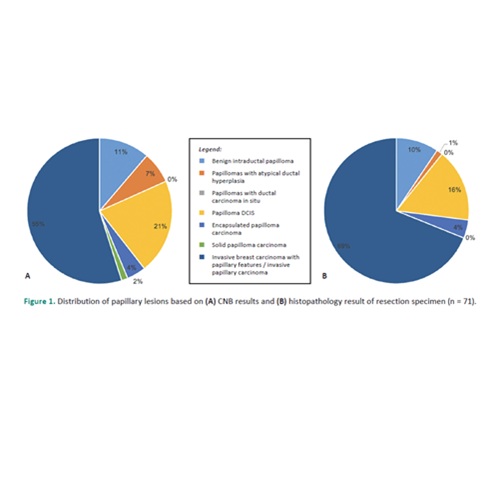
Methodology. A retrospective review of our institution’s database identified 184 papillary breast lesions diagnosed by core needle biopsy. The study population consisted of 71 samples that met the inclusion criteria. The overall upgrade and concordance rates were determined and analyzed if there was any significant association with clinical demographics, radiologic findings, and core diameter on gross examination. Continuous variables were presented as mean and median, and Shapiro-Wilk test was used to assess normality of data. Categorical variables were expressed as frequencies and percentages. Simple logistic regression analysis with Firth’s bias correction was performed to determine the variables associated with a diagnostic upgrade. P values ≤0.05 were considered statistically significant.
Results. A total 71 patients, all female, were included in the study. The overall upgrade rate was 8.45% (95% CI: 3.16-17.49%) in comparison with the diagnosis of the initial CNB and SE alone. This translated to 6/71 samples in this study. The overall concordance was 91.55% based on clinical significance, and an individual diagnosis concordance rate of 78.87%. None of the predictive factors (i.e., age, history of breast cancer, BI-RADS score, and gross core diameter) assessed showed an association with a diagnostic upgrade.
Conclusion. The computed overall upgrade rate is within range of currently published literature. The concordance rates for both clinical significance and individual diagnosis were quite high, suggesting good reproducibility of histopathologic diagnosis within our institution. This was also found to be consistent with other studies. Of the predictive factors, none showed an association to a diagnostic upgrade. Despite the latter, our findings may be of value within the medical center in further exploring and expanding the data set at hand, such that it may hopefully contribute to local guidelines in managing PBLs in the future.
Downloads
References
Salisbury T, Gurung A, Koonmee S, et al. Upgrade rate and predictive factors associated with breast papillary lesions on core biopsy: a Canadian experience. Int J Surg Pathol. 2023;31(7):1206-16. https://pubmed.ncbi.nlm.nih.gov/
https://doi.org/10.1177/10668969221137515
Kulka J, Madaras L, Floris G, Lax SF. Papillary lesions of the breast. Virchows Arch. 2022;580(1):65-84. https://pubmed.ncbi.nlm.nih.gov/34734332 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8983543 https://doi.org/10.1007/s00428-021-03182-7
WHO Classification of Tumours Editorial Board. WHO Classification of Tumours: breast
tumours, 5th ed, vol. 2. International Agency for Research on Cancer; 2019.
Brogi E, Krystel-Whittermore M. Papillary neoplasms of the breast including upgrade rates and management of intraductal papilloma without atypia diagnosed at core needle biopsy. Mod Pathol. 2021;34(Suppl 1):78-93. https://pubmed.ncbi.nlm.nih.gov/
https://doi.org/10.1038/s41379-020-00706-54
Qiu L, Mais DD, Nicolas M, Nanyes J, Kist K, Nazarullah A. Diagnosis of papillary breast lesions on core needle biopsy: upgrade rates and interobserver variability. Int J Surg Pathol. 2019;27(7):736-43. https://pubmed.ncbi.nlm.nih.gov/
https://doi.org/10.1177/1066896919854543
Hartmann LC, Sellers TA, Frost MH, et al. Benign breast disease and the risk of breast cancer. N Engl J Med. 2005;353(3):229-37. https://pubmed.ncbi.nlm.nih.gov/16034008 https://doi.org/10.1056/NEJMoa044383
Kim SY, Kim EK, Lee HS, et al. Asymptomatic benign papilloma without atypia diagnosed at ultrasonography-guided 14-gauge core needle biopsy: which subgroup can be managed by observation? Ann Surg Oncol. 2016;23(6):1860-6. https://pubmed.ncbi.nlm.nih.gov/ 26920388 https://doi.org/10.1245/s10434-016-5144-0
Genco IS, Tugertimur B, Manolas PA, Hasanovic A, Hajiveya S. Upgrade rate of intraductal papilloma without atypia on breast core needle biopsy: A clinical, radiological and pathological correlation study. Am J Surg. 2020;220(3):677-81. https://pubmed.ncbi.nlm.nih.gov/32007236 https://doi.org/10.1016/j.amjsurg.2020.01.040
Lin LH, Ozerdem U, Cotzia P, et al. Upgrade rate of intraductal papilloma diagnosed on core needle biopsy in a single institution. Hum Pathol. 2021;110:43-9. https://pubmed.ncbi.nlm.nih.gov/33159966 https://doi.org/10.1016/j.humpath.2020.10.012
MaColl C, Salehi A, Parpia S, Hodgson N, Ramonas M, Williams P. Benign breast papillary lesions diagnosed on core biopsy: upgrade rate and risk factors associated with malignancy on surgical excision. 2019;475(6):701-7. https://pubmed.ncbi.nlm.nih.gov/31372738 https://doi.org/10.1007/s00428-019-02626-5
Kılınç ANU, Bayramoğlu Z, Ünlü Y. Results of excision of unknown papillary neoplasms detected on core biopsy. Eur J Breast Health. 2021;17(3):258-64. https://pubmed.ncbi.nlm.nih.gov/34263154 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC8246050 https://doi.org/10.4274/ejbh.galenos.2021.6101
Nuñez D, Candanedo González F, Ibargüengoitia C. Papillary lesions of the breast: a review. 2020;9(4). https://doi.org/10.2217/bmt-2020-0028
Rubio IT, Wyld L, Marotti L, et al. European guidelines for the diagnosis, treatment and follow-up of breast lesions with uncertain malignant potential (B3 lesions) developed jointly by EUSOMA, EUSOBI, ESP (BWG) and ESSO. Eur J Surg Oncol. 2024;50(1):107292. https://pubmed.ncbi.nlm.nih.gov/38061151 https://doi.org/10.1016/j.ejso.2023.107292
The American Society of Breast Surgeons. Consensus guideline on concordance assessment of
image-guided breast biopsies and management of borderline or high-risk lesions. Columbia, MD,
Elfgen C, Leo C, Kubik-Huch RA, et al. Third International Consensus Conference on lesions of uncertain malignant potential in the breast (B3 lesions). Virchows Arch. 2023;483(1):5-20. https://pubmed.ncbi.nlm.nih.gov/37330436 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC10326140 https://doi.org/10.1007/s00428-023-03566-x
Kuehner G, Darbinian J, Habel L, et al. Benign papillary breast mass lesions: favorable outcomes with surgical excision or imaging surveillance. Ann Surg Oncol. 2019;26(6):1695-703. https://pubmed.ncbi.nlm.nih.gov/30737665 https://doi.org/10.1245/s10434-019-07180-7
Tay TKY, Tan PH. Papillary neoplasms of the breast-reviewing the spectrum. Mod Patjol. 2021;34(6):1044-61. https://pubmed.ncbi.nlm.nih.gov/33462367 https://doi.org/10.1038/s41379-020-00732-3
Rizzo M, Linebarger J, Lowe MC, et al. Management of papillary breast lesions diagnosed on core-needle biopsy: clinical pathologic and radiologic analysis of 276 cases with surgical follow-up. J Am Coll Surg. 2012;214(3):280-7. https://pubmed.ncbi.nlm.nih.gov/22244207 https://doi.org/10.1016/j.jamcollsurg.2011.12.005
Park SY, Ko SS, Yoon CS, Lee HK, Kang SS, Hur MH. Factors associated with disease upgrading in patients with papillary breast lesion in core-needle biopsy. Gland Surg. 2020;9(4):919-24. https://pubmed.ncbi.nlm.nih.gov/32953601 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7475353 https://doi.org/10.21037/gs-20-310
Bianchi S, Caini S, Vezzosi V, et al. Upgrade rate to malignancy of uncertain malignant potential breast lesions (B3 lesions) diagnosed on vacuum-assisted biopsy (VAB) in screen detected microcalcifications: Analysis of 366 cases from a single institution. Eur J Radiol. 2024;170:111258. https://pubmed.ncbi.nlm.nih.gov/38091661 https://doi.org/10.1016/j.ejrad.2023.111258
Lee SJ, Wahab RA, Sobel LD, et al. Analysis of 612 benign papillomas diagnosed at core biopsy: rate of upgrade to malignancy, factors associated with upgrade, and a proposal for selective surgical excision. AJR Am J Roentgenol. 2021;217(6):1299-311. https://pubmed.ncbi.nlm.nih.gov/34008998 https://doi.org/10.2214/AJR.21.25832
Zhang X, Liu W, Hai T, Li F. Upgrade rate and predictive factors for breast benign intraductal papilloma diagnosed at biopsy: a meta-analysis. Ann Surg Oncol. 2021;28(13):8643-50. https://pubmed.ncbi.nlm.nih.gov/34331160 https://doi.org/10.1245/s10434-021-10188-7
Foley NM, Racz JM, Al-Hilli Z, et al. An international multicenter review of the malignancy rate of excised papillomatous breast lesions. Ann Surg Oncol. 2015;22(Suppl 3):S385-90. https://pubmed.ncbi.nlm.nih.gov/26240010 https://doi.org/10.1245/s10434-015-4773-z
Li X, Weaver O, Desouki MM, et al. Microcalcification is an important factor in the management of breast intraductal papillomas diagnosed on core biopsy. Am J Clin Pathol. 2012;138(6):789-95. https://pubmed.ncbi.nlm.nih.gov/23161711 https://doi.org/10.1309/AJCPTDQCHIWH4OHM
Khan S, Diaz A, Archer KJ, et al. Papillary lesions of the breast: To excise or observe? Breast J. 2018;24(3):350-5. https://pubmed.ncbi.nlm.nih.gov/28845569 https://doi.org/10.1111/tbj.12907
Chen YA, Mack JA, Karamchandani DM, et al. Excision recommended in high-risk patients: Revisiting the diagnosis of papilloma on core biopsy in the context of patient risk. Breast J. 2019;25(2):232-6. https://pubmed.ncbi.nlm.nih.gov/30697873 https://doi.org/10.1111/tbj.13200
Chen P, Zhou D, Wang C, Ye G, Pan R, Zhu L. Treatment and outcome of 341 papillary breast lesions. World J Surg. 2019;43(10):2477-82. https://pubmed.ncbi.nlm.nih.gov/31209512 https://doi.org/10.1007/s00268-019-05047-2
Hong YR, Song BJ, Jung SS, Kang BJ, Lum SH, Chae BJ. Predictive factors for upgrading patients with benign breast papillary lesions using a core needle biopsy. J Breast Cancer. 2016;19(4):410-6. https://pubmed.ncbi.nlm.nih.gov/28053629 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5204047 https://doi.org/10.4048/jbc.2016.19.4.410
Alberty‐Oller JJ, Reyes S, Moshier E, et al. Does previous history of cancer or atypia predict histologic upgrade for pure intraductal papillomas diagnosed via core biopsy? A study of 490 cases at a single institution. Cancer Rep. 2021;5(3):e141. https://doi.org/10.1002/cnr2.1481.
Bernik SE, Troob S, Ying BL, et al. Papillary lesions of the breast diagnosed by core needle biopsy: 71 cases with surgical follow-up. Ann J Surg. 2009;197(4):473-8. https://doi.org/10.1016/j.amjsurg.2008.04.007
Tomlinson-Hansen SE, Khan M, Cassaro S. Breast Ductal Carcinoma in Situ. In: StatPearls. Treasure Island (FL): StatPearls Publishing; 2024. https://pubmed.ncbi.nlm.nih.gov/
Bookshelf ID: NBK567766
Petrolla A, Hicks DG, Skinner KA, Wang X. Detailed morphologic evaluation of breast papillary lesions on core biopsy is critical for accurate classification and clinical management: the experience of an Academic Institute. Clin Breast Cancer. 2022;22(4):e552-7. https://pubmed.ncbi.nlm.nih.gov/34998709 https://doi.org/10.1016/j.clbc.2021.12.004
Pinder SE, Shaaban A, Deb R, et al. NHS Breast Screening multidisciplinary working group guidelines for the diagnosis and management of breast lesions of uncertain malignant potential on core biopsy (B3 lesions). Clin Radiol. 2018;73(8):682-92. https://pubmed.ncbi.nlm.nih.gov/29773220 https://doi.org/10.1016/j.crad.2018.04.004
Glenn ME, Throckmorton AD, Thomison 3rd JB, Bienkowski RS. Papillomas of the breast 15 mm or smaller: 4-year experience in a community-based dedicated breast imaging clinic. Ann Surg Oncol. 2015;22(4):1133-9. https://pubmed.ncbi.nlm.nih.gov/25316488 https://doi.org/10.1245/s10434-014-4128-1
Youk JH, Kim EK, Kwak JY, Son EJ, Park BW, Kim SI. Benign papilloma without atypia diagnosed at US-guided 14-gauge core-needle biopsy: clinical and US features predictive of upgrade to malignancy. Radiology. 2011;258(1):81-8. https://pubmed.ncbi.nlm.nih.gov/20971773 https://doi.org/10.1148/radiol.10100728
Nakhlis F, Ahmadiyeh N, Lester S, Raza S, Lotfi P, Golshan M. Papilloma on core biopsy: excision vs. observation. Ann Surg Oncol. 2015;22(5):1479-82. https://pubmed.ncbi.nlm.nih.gov/25361885 https://doi.org/10.1245/s10434-014-4091-x
Pérez Fuentes JA, Marín Martínez CR, Ramírez Casadiego AK, Acosta Freites VF, Acosta Marín VA, Ruiz Castellano AC. Papillary breast lesions diagnosed by percutaneous needle biopsy: management approach. Ecancermedicalscience. 2019;13:902. https://pubmed.ncbi.nlm.nih.gov/30915160 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6390833 https://doi.org/10.3332/ecancer.2019.902
Elsharkawy M, Vestring T, Raatschen HJ. A ten-year, single-center experience: concordance between breast core needle biopsy/vacuum-assisted biopsy and postoperative histopathology in B3 and B5a cases. PLoS One. 2020;15(5):e0233574. https://pubmed.ncbi.nlm.nih.gov/32437426 https://www.ncbi.nlm.nih.gov/pmc/articles/PMC7241768 https://doi.org/10.1371/journal.pone.0233574
Ko D, Kang E, Park SY, et al. The management strategy of benign solitary intraductal papilloma on breast core biopsy. 2017;17(5):367-72. https://pubmed.ncbi.nlm.nih.gov/28438672 https://doi.org/10.1016/j.clbc.2017.03.016
Moseley T, Desai B, Whitman GJ, et al. Benign breast intraductal papillomas without atypia at core needle biopsies: is surgical excision necessary? Ann Surg Oncol. 2021;28(3):1347-55. https://pubmed.ncbi.nlm.nih.gov/32860176 https://doi.org/10.1245/s10434-020-09061-w
Ahn SK, Han W, Moon HG, et al. Management of benign papilloma without atypia diagnosed at ultrasound-guided core needle biopsy: Scoring system for predicting malignancy. Eur J Surg Oncol. 2018;44(1):53-8. https://pubmed.ncbi.nlm.nih.gov/29174198 https://doi.org/10.1016/j.ejso.2017.10.214
Downloads
Published
How to Cite
Issue
Section
License
Copyright (c) 2025 Manuelito Madrid, Nicole Dominique Santos

This work is licensed under a Creative Commons Attribution-NonCommercial-ShareAlike 4.0 International License.









 @philippinepathologyjournal
@philippinepathologyjournal